|
Organ-sharing agencies assign these patients an artificial score according to the number and size of tumours, providing them access to liver transplantation within a maximum of 18 months. (3) Those with HCC on compensated liver cirrhosis. 
Those with very high MELD score may likely access liver transplantation within days or a few weeks, whereas those with intermediate or low MELD scores will access liver transplantation within months or even years. (2) Those with decompensated liver cirrhosis, included in the waiting list on the principle of the ‘sickest first’, based mainly on the calculation of the Model for End Stage Liver Diseases (MELD) score. (1) Those with acute liver failure, included, in most countries, in a super-emergency waiting list giving them absolute priority over all other recipients, and receiving a transplant within hours or days. The waiting lists for liver transplantation are composed of three types of patient. Therefore, the wait for transplantation can vary from a few days in the case of acute liver failure patients to more than 1 year for patients with cirrhosis of intermediate severity or those with HCC. In contrast to living donor transplantation, where the date of liver transplantation is known in advance, in cadaveric donor liver transplantation the date of liver transplantation is unknown. In Europe, liver donors are mainly of cadaver origin, either following brain death or cardiac arrest, under the Maastricht 3 procedure. Such success comes as a consequence of the absence of alternative therapies and of the good post-transplant survival of approximately 90 and 80% at 1 and 5 years, respectively. The success of liver transplantation over the past years has been considerable, with more than 5000 being performed annually in Europe, surmounting to more than 140,000 liver transplantations in total. It concerns all patients with end-stage liver disease when other medical therapies have failed as well as a high number of patients with primary liver cancer, mainly hepatocellular carcinoma (HCC). Liver transplantation plays a major role in the therapeutic path of liver diseases. The management of patients on the waiting list is an essential component of the success of liver transplantation. There is a diversity of patients on the waiting list for transplantation and equity should be preserved between those with cirrhosis of high and intermediate severity and those with HCC. For patients with cirrhosis and intermediate MELD score, waiting time can exceed 1 year therefore, regular follow-up and management are essential to maintain the patient alive on the waiting list and to achieve a good survival after liver transplantation. For patients with HCC, a bridge therapy is frequently required to avoid progression of HCC and to maintain patients within the criteria of liver transplantation as well as to reduce the risk of post-transplant recurrence of HCC. 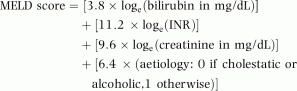
It is also essential to identify the ideal timing for liver transplantation in order to minimise mortality rates. For the more severe cases who may swiftly access liver transplantation, it is essential to rapidly determine whether liver transplantation is indeed indicated, and to organise a fast workup ahead of this. The management of patients on the waiting list is of prime importance to avoid death and drop out from the waiting list as well as to improve post-transplant survival rates. For this latter group of patients, ‘MELD exception’ points can be arbitrarily given. These criteria can lead to a ‘competition’ on the waiting list between the above patients and those who are cirrhotic and have an intermediate MELD score or with life-threatening liver diseases not well described by the MELD score. Generally, priorities are given to cirrhotic patients with a high Model for End-Stage Liver Disease (MELD) score on the principle of the sickest first and to patients with hepatocellular carcinoma (HCC) on the principle of priority points according to the size and number of nodules of HCC. The success of liver transplantation has led to an increase in the indications for liver transplantation. The results of liver transplantation are excellent, with survival rates of over 90 and 80% at 1 and 5 years, respectively.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
